AMH (Anti Muller Hormone)
AMH from serum: this test shows the current status of fertility.
Predict the onset of your menopause
With a one-time measurement of the Anti-Müller-Hormone (AMH) in the blood, the age at which a woman reaches menopause can be estimated fairly accurately. This was reported by researchers from the University of Medical Science in Tehran at the congress of the European Society of Human Reproduction and Embryology in Rome. The researchers, led by Fahimeh Ramezani Tehrani, took blood samples from 266 women aged between 20 and 49 who were already taking part in the Tehran Lipid and Glucose Study three times at three-year intervals from 1998 onwards to measure the Anti-Müller Hormone (AMH). In addition, the women received a physical examination every three years and the researchers collected data on socioeconomic status and reproductive history.
Please note that this test measures the AMH value. The lab report does not include a personal prediction of exactly when you will enter menopause.
Estimate
Ramezani Tehrani developed a statistical model to estimate menopausal age from a single measurement of AMH concentration. She applied this model to the AMH concentrations measured at different points in the women's reproductive lives. The estimate corresponded well with the actual outcome in 63 women who reached menopause during the study: the difference was at most four months.
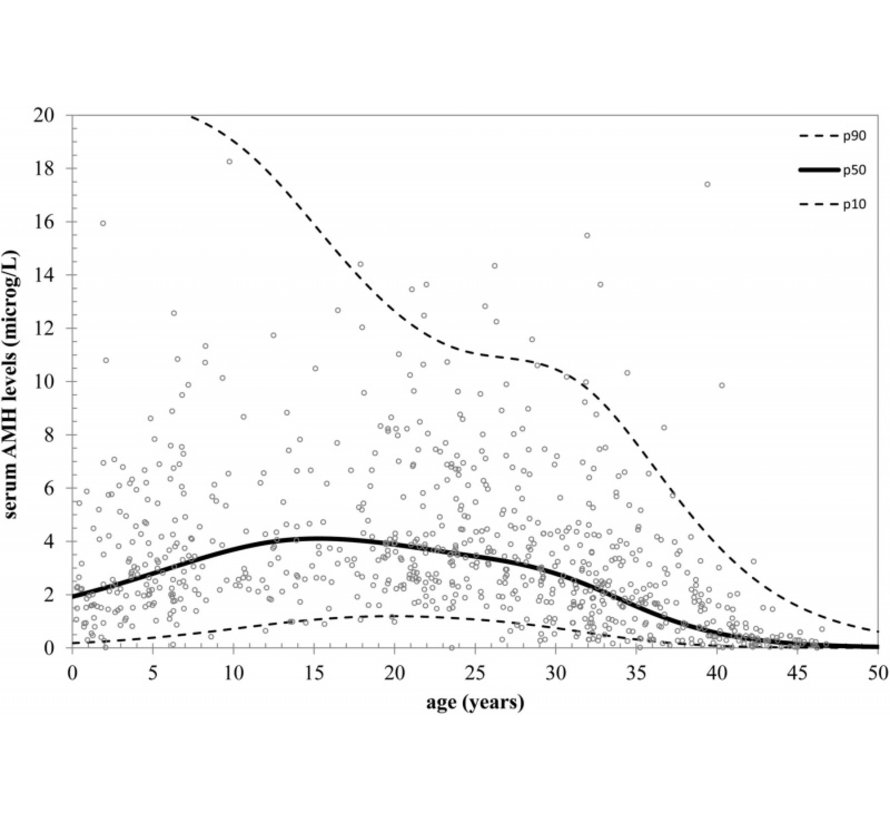
Normal Values
At different ages, Ramezani Tehrani established a kind of limit for the concentration of AMH that indicates early (under 45) or late (over 50) menopause. The AMH concentration indicative of early menopause is a maximum of 4.1 ng/ml 3.3 ng/ml and 2.4 ng/ml in women aged 20, 25 and 30 years, respectively. For late menopause, AMH concentration should be at least 4.5 ng/ml, 3.8 ng/ml and 2.9 ng/ml in these three age groups.
Family Planning
According to Ramezani Tehrani, this study is the first prediction of menopausal age to come from a population-based study. "We believe that our estimates of menopausal age based on AMH concentrations are sufficiently valid for practicing physicians to assist women with their family planning. A realistic estimate of reproductive status can be made well before menopause is reached. For example, if a woman in her 20s has a serum concentration of 2.8 ng/ml, we think she will reach menopause between the ages of 35 and 38. "
Ramezani Tehrani acknowledges that her study is still small in scope. The results will need to be confirmed in a larger study with longer follow-up.
AMH levels in women
- In the fertile phase, the result is between 1.0 and 8.0 ng/ml
- With impaired fertility, the result is between 0.4 and 1.0 ng/ml
- In an infertile phase the measured value is lower than < 0.1 ng/ml
- If the result is higher than 8, there may be PCOS.
PCOS
PCO-S stands for poly cystic ovarian syndrome. On ultrasound image, many small cysts can be seen in the ovary.
The diagnosis is made by 2 of the following 3 symptoms:
- First, ovulation problems, which means less often or no ovulation.
- Second is an excess of male hormone.
- Third, a typical ultrasound image many small cysts in the ovary.
PCOS is a complicated hormonal disorder. Health problems occur in varying degrees and in different areas. Often there are problems with getting pregnant. But there are also problems in the metabolism of fats and on a psychological level. PCOS occurs in 10 to 12% of women.
The hormones that control the ovaries (ovaries) are out of balance in PCOS. FSH, Follicle stimulating hormone, causes eggs to grow in ovaries. LH, Luteinizing hormone is the hormone that makes the egg jump. In PCOS, the LH is continuously higher than the FSH. As a result, no egg matures, no ovulation occurs and there is no chance of pregnancy.
The metabolism is different in PCOS patients. This is reflected in a wrong balance of fats. The unhealthy fats LDL and cholesterol are increased compared to the healthy fats HDL. Often the sugar metabolism is also different. There is a tendency toward type II diabetes.
Due to an excess of male hormones (hyper androgenism) there are complaints of excessive hair growth, acne and baldness.
The altered metabolism also causes obesity and an increased risk of cardiovascular disease.
Complaints of stress are more common in PCOS patients. Relative to women who do not have PCOS, depression is 4 times more common and anxiety symptoms are 6 times more common.
Not every woman with PCOS is at the same health risk, so not every woman with PCOS needs the same treatment or preventive measures. The individual health risk depends on the PCOS type and environmental factors such as age.
Patients are advised to lose weight. And that is difficult. But a downward trend is already good. This leads to a different and better balance of hormones. Treatment to induce ovulation is then also easier.
With regard to fertility problems, it is important to have an ovulation. This can be induced with clomiphene citrate tablets. Shortly after menstruation, a tablet of clomiphene citrate is taken for 5 days. The brain then thinks that the ovaries are not working. As a result, the brain makes more FSH which prompts the ovaries to mature an egg.
When this does not result in ovulation, the administration of FSH is used. This can only be administered via injections. The effect of this treatment must also be monitored much more closely with ultrasound scans. The FSH is either purely replicated or extracted from urine of women with young pregnancies (mothers for mothers).
If it is successful in inducing a regular ovulation, there are, by having regular sexual intercourse, chances of a pregnancy. If a pregnancy is not achieved, insemination (introducing semen directly into the uterus) may be necessary. If pregnancy is still not achieved, test tube fertilization may be used.
People with PCOS do well to maintain a healthy lifestyle. In addition, when you see your doctor, you should consider talking about your individual risk of developing cardiovascular disease.